🔍
Created date
TitleCreated dateModified dateMenu OrderRandomNumber of commentsPost InSort By None
4Sight Communications named a supplier on Crown Commercial Service’s Network Services 3 agreement (RM6116)
4Sight Communications, a CloudClevr company, are proud to announce that it has been named as...
Mitel recognises 4Sight as their Enterprise Partner of the Year
4Sight Communications recently won the Mitel Enterprise UK&I Partner of the Year award...
4Sight support Heathfield & Waldron RFC’s Under 15s tour to Jersey
Grass roots rugby prides itself on being an inclusive sport, built on the core values...
4Sight become a G-Cloud 13 supplier
4Sight Communications are proud to announce our appointment as a G-Cloud 13 supplier for the...
4Sight extends its as a service portfolio to include 8×8 and RingCentral
As the communications landscape shifts towards hybrid working, customers are looking to engage with organisations...
Mitel and RingCentral partner to dominate the cloud communication space
Customers accepted reduced service as companies shifted to working from home, but now expect a...
Report | Hybrid Working 2021
Customers accepted reduced service as companies shifted to working from home, but now expect a...
4Sight Communications awarded Mitel Platinum status
4Sight Communications awarded Mitel Platinum status 4Sight Communications, having already been recognised through the Mitel...
MITEL UC PROMOTIONS Q3 2019
MITEL UC PROMOTIONS Q3 2019 MAKE THE MOVE TO A MIVOICE PLATFORM BUY 3...
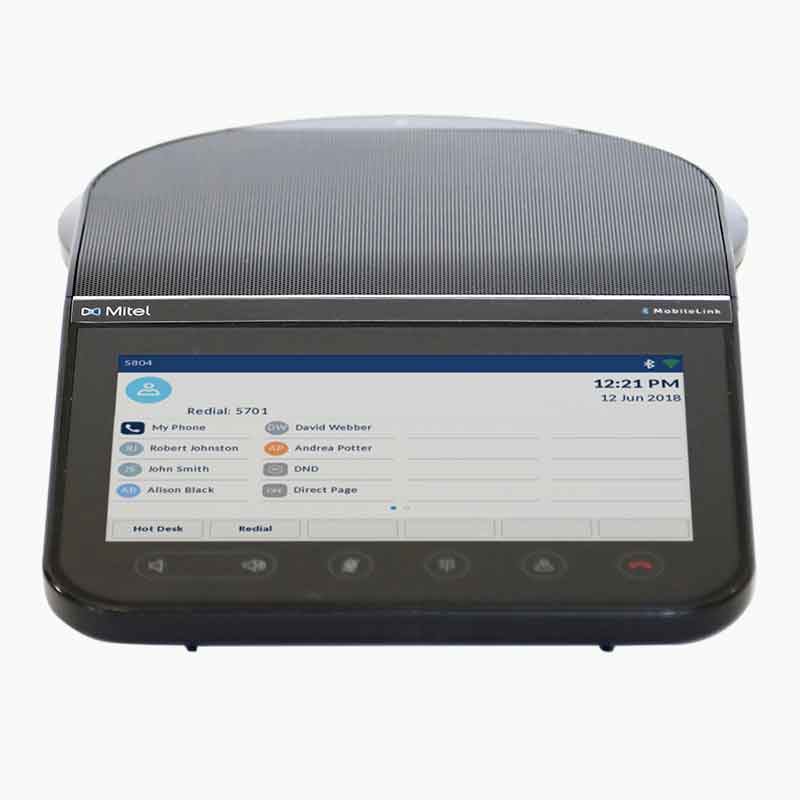
Introducing the new Mitel 6970 IP Conference Phone
The new Mitel 6970 IP Conference Phone is available for MiVoice Business. The Mitel 6970...
4Sight Crowned Mitel´s ‘Top Services Partner’ Of The Year
4Sight Communications Awarded ‘Top Services Partner’ at Mitel's Next '2019 International Partner Awards'We are extremely...
Avaya End of Support for the CS1000
As of April 2019, Avaya is officially ending the support for the release 7.6 and...